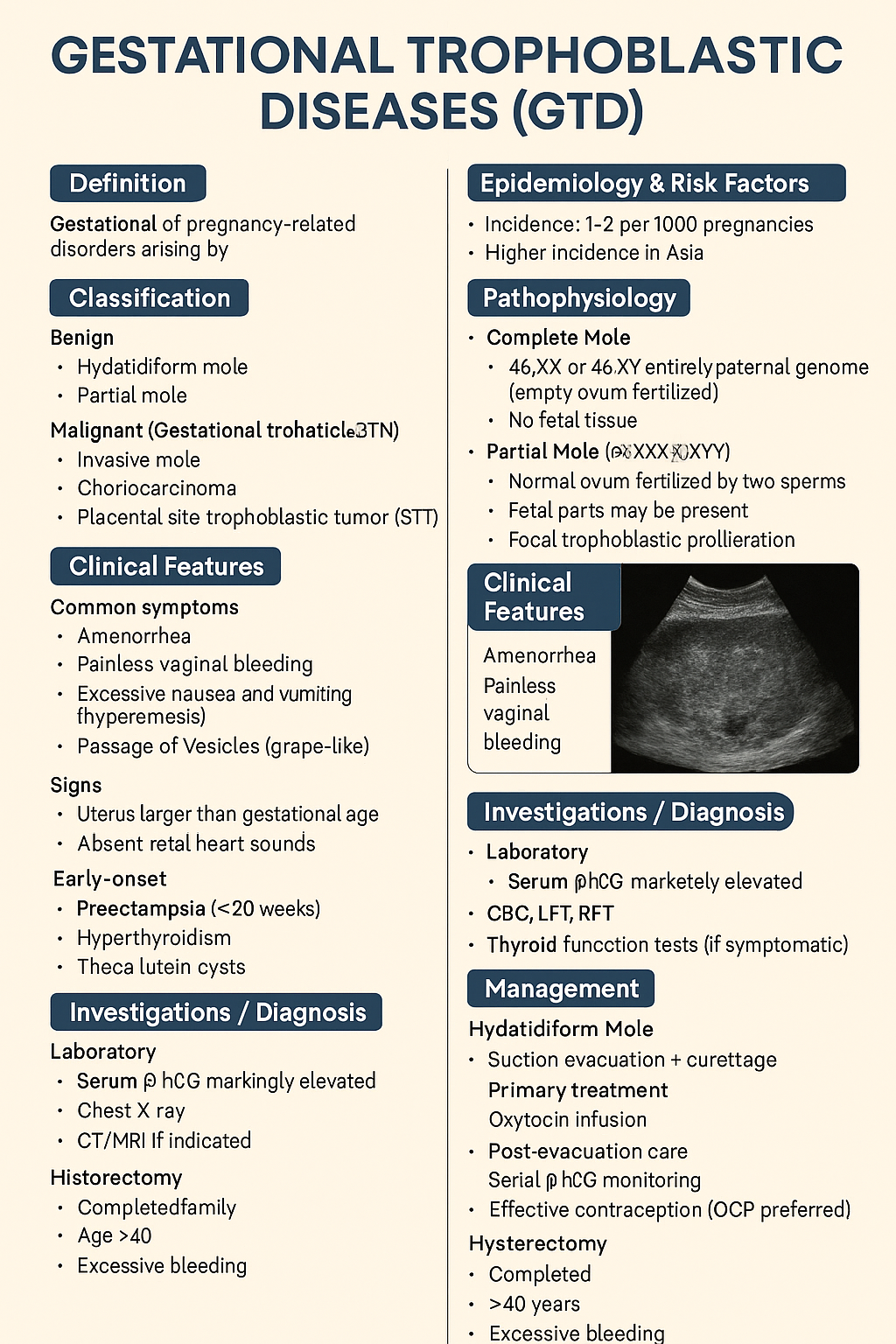
Gestational Trophoblastic Disease Explained: Complete Guide for Diagnosis, FIGO Staging and Treatment
Below is a **single-place, comprehensive, exam-oriented + clinical reference** on **Gestational Trophoblastic Diseases (GTD)**, structured exactly for **medical study, practice, and management**.
---
# **Gestational Trophoblastic Diseases (GTD)**
## **Definition**
Gestational Trophoblastic Diseases are a **spectrum of pregnancy-related disorders** arising from **abnormal proliferation of trophoblastic tissue** (placental tissue). They range from **benign hydatidiform mole** to **malignant gestational trophoblastic neoplasia (GTN)**.
---
## **Classification**
### **1. Non-neoplastic GTD**
* **Complete hydatidiform mole**
* **Partial hydatidiform mole**
### **2. Gestational Trophoblastic Neoplasia (GTN)**
* **Invasive mole**
* **Choriocarcinoma**
* **Placental site trophoblastic tumor (PSTT)**
* **Epithelioid trophoblastic tumor (ETT)**
---
## **Epidemiology**
* Incidence: **1–2 per 1000 pregnancies**
* Higher in:
* Extremes of maternal age (<15, >40)
* Prior molar pregnancy
* Asian populations
* Recurrence risk:
* After one mole: **1–2%**
* After two moles: **15–20%**
---
## **Pathophysiology & Genetics**
### **Complete Mole**
* **46XX or 46XY**
* Entirely paternal genome (androgenesis)
* Empty ovum fertilized by sperm → duplication
* **No fetus**
### **Partial Mole**
* **Triploid (69XXX/XXY/XYY)**
* Two sperms fertilize one ovum
* **Abnormal fetus may be present**
---
## **Clinical Features**
### **Symptoms**
* Amenorrhea
* Vaginal bleeding (most common)
* Excessive vomiting (hyperemesis gravidarum)
* Early-onset preeclampsia (<20 weeks)
* Hyperthyroid symptoms (↑ β-hCG)
* Passage of grape-like vesicles (rare)
### **Signs**
* Uterus larger than gestational age (complete mole)
* Absent fetal heart sounds
* Bilateral theca-lutein ovarian cysts
---
## **Investigations / Diagnosis**
### **Laboratory**
* **β-hCG**:
* Markedly elevated (often >100,000 IU/L)
* Thyroid function tests (rule out thyrotoxicosis)
* CBC (anemia)
* Liver, renal function tests
* Blood group & Rh typing
### **Imaging**
* **Ultrasound (gold standard)**
* Complete mole: *“Snowstorm / cluster of grapes”*
* Partial mole: fetus + cystic placenta
* Chest X-ray (baseline for metastasis in GTN)
### **Histopathology**
* Definitive diagnosis after evacuation
---
## **Differential Diagnosis**
* Missed abortion
* Multiple pregnancy
* Ectopic pregnancy
* Placental mesenchymal dysplasia
* Subchorionic hemorrhage
---
## **Management**
### **Initial Management of Hydatidiform Mole**
#### **1. Uterine Evacuation**
* **Suction evacuation + curettage (preferred)**
* Oxytocin infusion after evacuation
* Hysterectomy (if completed family + >40 yrs)
#### **2. Anti-D Immunoglobulin**
* For Rh-negative women
---
## **Post-Evacuation Follow-Up**
### **β-hCG Monitoring**
* Weekly until **normal for 3 consecutive weeks**
* Then monthly for:
* **6 months (partial mole)**
* **12 months (complete mole)**
### **Contraception**
* Mandatory during follow-up
* Combined oral contraceptives are safe
---
## **Gestational Trophoblastic Neoplasia (GTN)**
### **Diagnostic Criteria (FIGO)**
* Plateauing β-hCG (±10% for 4 values over 3 weeks)
* Rising β-hCG (>10% for 3 values over 2 weeks)
* Persistently detectable β-hCG >6 months
* Histological choriocarcinoma
---
## **FIGO Staging**
| Stage | Description |
| ----- | ------------------------------- |
| I | Confined to uterus |
| II | Extends to pelvis |
| III | Lung metastasis |
| IV | Other metastasis (brain, liver) |
---
## **WHO Risk Scoring**
Low risk: **0–6**
High risk: **≥7**
---
## **Chemotherapy**
### **Low-Risk GTN**
**Single-agent chemotherapy**
#### **Methotrexate**
* **Indication:** Low-risk GTN
* **Mechanism:** Folate antagonist → inhibits DNA synthesis
* **Dose:**
* 50 mg IM weekly OR
* 0.4 mg/kg/day × 5 days
* **Adverse effects:** Stomatitis, hepatotoxicity, myelosuppression
* **Contraindications:** Liver disease, renal failure
* **Monitoring:** LFTs, CBC
* **Counselling:** Avoid alcohol, pregnancy
OR
#### **Actinomycin-D**
* **Mechanism:** DNA intercalation
* **Dose:** 1.25 mg/m² IV every 2 weeks
* **Adverse effects:** Alopecia, nausea
---
### **High-Risk GTN**
**Multi-agent chemotherapy**
#### **EMA-CO Regimen**
* **Etoposide**
* **Methotrexate**
* **Actinomycin-D**
* **Cyclophosphamide**
* **Vincristine**
**Indication:** WHO score ≥7
**Cure rate:** >90%
---
## **Specific GTN Types**
### **Choriocarcinoma**
* Highly malignant
* Early hematogenous spread (lungs, brain)
* Very high β-hCG
* Extremely chemosensitive
### **PSTT / ETT**
* Low β-hCG
* Less chemosensitive
* **Primary treatment: hysterectomy**
---
## **Complications**
* Hemorrhage
* Thyrotoxicosis
* Pulmonary embolism
* Metastasis (lung, brain, liver)
* Chemotherapy toxicity
---
## **Prognosis**
* Overall cure rate: **>95%**
* Fertility preserved in most cases
* Future pregnancies usually normal
---
## **Patient Counselling**
* Excellent prognosis with treatment
* Strict β-hCG follow-up is life-saving
* Contraception essential during follow-up
* Recurrence risk low but real
---
If you want next:
* **High-yield MCQs (case-based)**
* **FIGO scoring calculator**
* **Flowchart-style management**
* **HTML/CSS/JS exam notes page**
* **Differentiation table (mole vs choriocarcinoma)**
Just tell me 👍